This Might Be The Reason Your Acne Won't Go Away
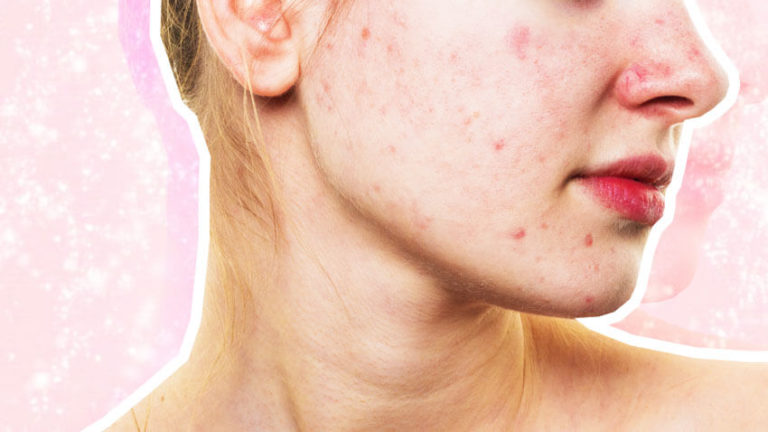
If you feel as if you’ve tried every acne treatment on the shelves, and nothing has worked, then it might be because you don’t have ‘traditional acne’. What you may have determined as acne, may actually be Malassezia folliculitis, which is more commonly known as fungal acne. And while it may look similar, it needs to be treated differently, as ordinary acne treatments could aggravate the breakout. For the 411 on fungal acne, we spoke to Founder of Dr. Dennis Gross Skincare, Dr. Dennis Gross, who told us everything from how to treat fungal acne to how to avoid it…
What causes fungal acne?
“’Fungal acne’ is actually called Malassezia folliculitis (or pityrosporum folliculitis). It’s an infection caused by excess yeast that aggravates your hair follicles. Yeast can feed on the oil found in your skin, making oilier skin and oilier skin areas more prone to developing an infection,” Dr. Dennis told us.
When we asked Dr. Gross what increases the likelihood of having fungal acne, he explained; “Oilier skin types may be more prone to fungal acne. Using oil-based products that throw your skin off balance could also increase your risk of developing fungal acne. There are also environmental factors like heat and humidity that will amp up the likelihood of an infection, as well as if you’re someone who sweats more.”
If you’re someone who has a tendency to get fungal skin conditions, like seborrheic dermatitis or dandruff, then consider yourself a more likely candidate.
How do you distinguish between regular acne and fungal acne?
Dr. Gross states, “As mentioned above, fungal acne is really Malassezia folliculitis. It may look like hormonal or bacterial acne, but it refers specifically to excess yeast that’s built up in your hair follicles, causing breakout-like symptoms. It’s not actually ‘acne’ but an infection in your hair follicle. In terms of how to spot the difference on yourself, you’ll find classic acne on your face, generally in the T-zone, on the jawline and on the cheeks. You’ll find ‘fungal acne’ more on your chest and upper back and the spots will look more consistent in terms of size. Fungal acne will come with more of an itching feeling.” Large cysts, blackheads, and whiteheads are not fungal related, so if you’re experiencing any of these types of pimples or a combination of them, it is most likely not fungal acne.
“There may sometimes be overlap in ingredients that alleviate infections, but this will go case by case and the two should largely be addressed and treated differently. For example, as I mentioned above, sulfur is both anti-fungal and anti-bacterial so could be used to treat both conditions. However, there are also some treatments that may kill the wrong bacteria (the normal kind on your skin that may be helping to fight the yeast) making pityrosporum folliculitis worse.”
Posts You'll Love:
How to treat fungal acne like a derm
“Treatments can vary from incorporating sulfur into your skincare routine (it is both anti-fungal and anti-bacterial) to needing an anti-fungal oral medication prescribed, it all depends on the severity of your infection and the frequency of it. Salicylic acid is another helpful ingredient. You can also incorporate an oil-free moisturizer like the Dr. Dennis Gross Hyaluronic Marine Oil-Free Moisture Cushion, $60, into your routine to limit the oil that yeast can feed on.”
Products to treat Malassezia folliculitis:
 Source: Bioderma
Source: Bioderma
Bioderma Sebium H2O Micellar Water, $15: This micellar water contains anti-fungal powerhouse, sulfur, making it the perfect first step of your nighttime routine. Not only will it help the infection, but it’ll also help balance oil production while removing your makeup.
 Source: Neutrogena
Source: Neutrogena
Neutrogena Body Clear Body Wash, $8: If you’re prone to fungal acne on your chest or back, this product should be at the top your list. The formula contains 2% salicylic acid; a potent BHA that’ll exfoliate the skin and dissolve the glue that binds dead skin cells, which block your pores. It’ll also help lower oil production, and as it has anti-inflammatory properties it’ll soothe existing spots. Once you’ve massaged it onto damp skin, massage it in for one minute.
 Source: Nizoral
Source: Nizoral
Nizoral A-D Anti-Dandruff Shampoo, $14: This anti-fungal shampoo is often prescribed to treat bad cases of dandruff and seborrheic dermatitis as it kills the fungal growth. Apply a dime-sized amount to the area and let it sit for two minutes before rinsing. You can also use other anti-dandruff shampoos like Selsun Blue or those that contain ketoconazole.

Try BHAs: The Inkey List BHA serum, $11, is packed with salicylic acid, which will help exfoliate pores and fight fungal breakouts.
What to avoid if you have fungal acne…
“Avoid keeping sweaty workout clothes on post-workout and be mindful of settings (like a locker room) where you’re more likely to encounter yeast. You’ll also want to be sure to cleanse and stay dry when in more humid environments” explains Dr. Gross. If you’re prone to fungal acne, you may also want to decrease the amount of sugar in your diet, as the yeast bacteria thrive on sugar. Ultimately, if you’re unsure, go and see your doctor or derm, who will be able to help you decide and plan the best course of treatment.
For more info on how to soothe and calm other acne types, check out our ultimate skincare guide to acne.




















Leave a comment