How Lupus Affects Your Skin and Body – Plus, How to Manage It
 Source: Tibrina Hobson/Getty Images
Source: Tibrina Hobson/Getty Images
Roughly five million people across the world are currently living with lupus – and of those millions 90% are women(I). This chronic autoimmune disease affects people in many different ways. For example, one form of lupus only affects your skin, while another form can affect your body’s major organs and tissues. Symptoms can range from hair loss to skin rashes, from cognitive issues to physical impairments.
It’s important to note that lupus is still a relatively confounding disease that experts and doctors are striving to understand better every day. With that said, our knowledge of lupus – and the way it impacts the body – has truly grown since it was discovered in 1948. You may have heard about lupus on social media or in the news thanks to pop star Selena Gomez, who also has Lupus and has been raising awareness about the disease. In fact, in 2017 Selena had to have a kidney transplant due to symptoms caused by lupus.
To help fill you in on what we do know about lupus, we spoke to a handful of medical experts. By absorbing this information, we hope you’ll be able to better understand and manage lupus or perhaps be able to spot signs that could help someone else get checked out.
So, What Exactly is Lupus?
As we alluded above, lupus is a super complex disease that the medical community is valiantly working to untangle. That said, Dr. Matthew Kohler – a double board-certified medical doctor and co-founder of New York City’s Ospina Medical – gave us the general gist.
“Lupus is a chronic autoimmune disease where the body’s immune system has difficulty differentiating between your own normal healthy cells and foreign cells,” he explains. “[The disease causes your body to] begin attacking healthy tissue, leading to widespread inflammation and pain.”
He goes on to explain that lupus can affect a variety of organs in your body, including your skin, heart, blood vessels, brain, kidney, joints, bones, and lungs. How and what it attacks, though, depends on which of the four forms of lupus you’ve been diagnosed with.
The Four Types Of Lupus
The four types of lupus include systemic lupus erythematosus (SLE), cutaneous lupus, drug-induced lupus, and neonatal lupus(II). That’s a lot of medical jargon, so let’s break it down for you.
Systemic Lupus Erythematosus (SLE)
This is the most common form of lupus, accounting for roughly 70% of all cases. It manifests in a range of very mild to severe symptoms.
“[For example, it can present as] inflammation of the kidneys, causing alterations in your body’s ability to filter waste from the blood. [Or it can present as] inflammation of the nervous system and brain causing memory change, confusion, headaches or even stroke,” says Dr. Rajivan Maniam, who’s double board-certified in anesthesiology and pain medicine. “[This form of lupus can also present as] inflammation of the brain’s blood vessels, causing high fevers, seizures or behavior changes, and even coronary artery disease due to buildup of deposits in the artery walls.”
Drug-Induced Lupus
As the name implies, this form of lupus is directly caused by certain medications. It accounts for roughly 10% of all cases and presents similarly to SLE lupus.
“Although specific criteria for this form of lupus has not officially been established, many of the symptoms overlap with SLE, including muscle and joint pain with swelling, flu-like symptoms and [tissue inflammation],” notes Dr. Maniam.
Once medications are stopped, the symptoms typically subside. Dr. Maniam says that common drugs connected to drug-induced lupus include hydralazine (which is used to treat hypertension), procainamide (used to treat cardiac arrhythmias), and isoniazid (used in tuberculosis treatment). It’s important to maintain heightened communication with your doctor when taking these, and other, medications.
Neonatal Lupus
Neonatal lupus is an exceptionally rare form of lupus that infects infants. Neonatal lupus is typically already present at birth, and it is sometimes even discovered while the baby is still in the womb(III). During pregnancy, neonatal lupus can present as a slower-than-usual heartbeat. Once delivered, Dr. Maniam says that sick infants may show symptoms of a skin rash, liver problems, or low blood cell counts. Fortunately, these symptoms tend to improve within six months’ time.
Cutaneous Lupus
Also referred to as discoid lupus, this form of lupus impacts only your skin. It accounts for approximately 10% of cases.
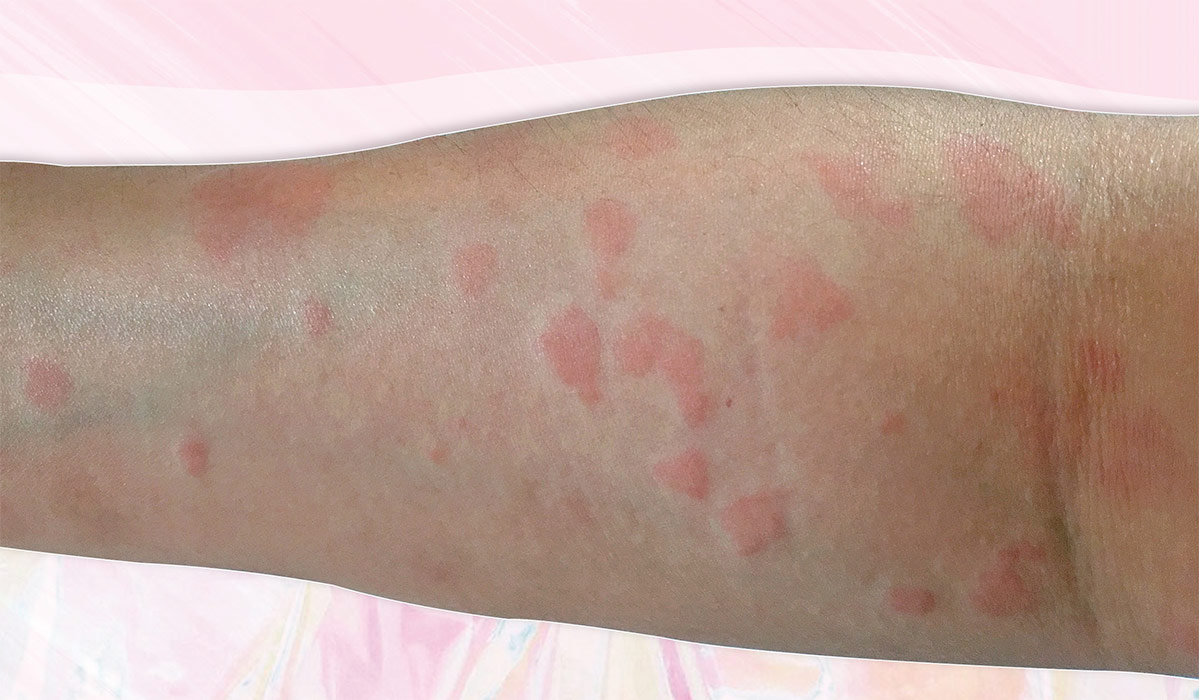
“Cutaneous lupus is the skin presentation [of lupus] that causes rashes or sores (lesions) throughout the body. Many of the lesions will appear on high sun-exposure areas of the body such as the face, neck and ears, scalp, arms or legs,” explains Dr. Ava Shamban, a board-certified dermatologist with clinics in Santa Monica and Beverly Hills, California. “Nails may become inflamed, as well, in the under-tissue. This can cause cracking, swelling or bubbling, spotting, redness, and soreness.”
The good news is that these round lesions which are typically red, scaly, and thick – generally do not cause pain. However, it’s important that they are managed and treated since, over time, they can create scar tissue. (We’ll dive into lupus treatment in a second, but spoiler alert: never forget to wear your SPF.)
“This same type of discoid lesion can also occur on the scalp and may cause the hair to fall out,” adds Dr. Shamban. “Part of this is the disruption to the follicle area and its ability to perform production to push the hair through the scalp. However, it is also the process of telogen effluvium where a traumatic cellular, emotional, physical, or other types of illness will stop the growth phase of the hair and put it into the resting phase where patients will see the shedding.”
This type of shedding is typically temporary, and your hair will grow back. However, if the lesions form scars when they heal then the hair loss may be permanent. Again, it’s important to manage these lesions.
How Does Someone Get Lupus?
The onset of lupus can be caused by both genetic and outside factors, notes Dr. Maniam. Some people have an inherited genetic predisposition, which means they have a higher likelihood of triggering lupus since members of their family had it. For others, lupus can be triggered by environmental stressors, including sunlight, infections, and medications.
As mentioned above, women are also more likely to develop lupus – particularly those between ages 15 and 45. Certain races are more prone to developing lupus, as well, including Black, Hispanic, and Asian people.
Posts You'll Love:
How Is Lupus Diagnosed?
Remember the part where we mentioned that lupus is super complex, and that research is underway? Those factors definitely impact diagnoses. If you’ve ever watched an episode (or two) of the TV show, House, they often allude to this. What we’re saying is that it isn’t always cut-and-dry.
“Lupus can sometimes be difficult to diagnose, as it mimics other ailments,” explains Dr. Kohler. “[However], the most distinctive presentation of lupus is identifying a facial rash in the shape of butterfly wings across both cheeks, in medical terms called a malar rash.’”
 Source: WedMD
Source: WedMD
He adds that signs and symptoms of lupus also depend on which part of the body is being infected. Outside of the visible sign of the butterfly rash, other symptoms include persistent fatigue, fever, joint pain, joint stiffness, and swelling. For some, it presents as shortness of breath, chest pain, dry eyes, headaches, memory loss, and even white/blue fingers and toes.
“In order to assist your doctor to find out if you have lupus, it is important to give a thorough medical history of your symptoms [and] indicate any family history of lupus or other autoimmune diseases,” says Dr. Maniam. “[You should also] complete a full physical exam, complete a skin or kidney biopsy, blood test, and urine test that would indicate if you have the autoantibodies that attack your healthy cells.”
Since lupus can range from having mild to life-threatening symptoms, getting an early diagnosis, and managing the disease well, is super important(IV). Dr. Maniam says that early diagnosis is often done by a rheumatologist – AKA a specialist who’s trained and experienced with the treatment of arthritis, lupus, and other joint, muscle, and bone diseases. This person can help come up with a lupus management plan, as well.
How To Manage Lupus – Including Skin Lesions
Working closely with a doctor to manage your lupus is vital to your health. They might also prescribe you certain medications that ease discomfort and help your body work more as it should. That said, there are some things you can do at home, including lifestyle changes, that can help, as well.
Posts You'll Love:
Inside-Out Care
For example, Dr. Kohler says that patients with lupus can take over-the-counter NSAIDs such as ibuprofen and high-dose aspirin – to treat things like fever, arthritic pain, and inflammation (speak with your doctor first.) Also, simply caring for your body can do wonders, too.
“Proper treatment and lifestyle management will significantly improve the overall quality of life for patients with lupus. It is important to stay physically active, keep healthy diets, [and] rest,” says Dr. Kohler. “In general, nutritious and well-balanced diets from all the food groups is important.”
There’s no magic “cure-all” diet for lupus. Rather, aim to eat lots of colorful fruits and vegetables, lean meats such as chicken and fish, and whole grains(V). And BTW, if you do take any supplements or vitamins, run them by your doctor first to make sure they won’t interfere with any of your current medications.
Skincare
As for lupus skincare, there are a few things you can do. Number one – and this is key – is to really watch your time spent in the sun, stresses Dr. Shamban. When your skin is exposed to the sun’s UV rays, lesions can develop or worsen.
You should apply an SPF 30+ every single day – even when it’s raining, even in the winter, and even when you’re indoors. Reapply every two hours if you’re outdoors (or if you’ve gotten wet/sweated) and every four hours if you’re inside. Also, do your best to avoid the sun during prime hours, which is 10 a.m. to 2 p.m.
 Source: Versed, Sun Bum
Source: Versed, Sun Bum
For facial care, we like Versed Guards Up Daily Mineral Sunscreen Broad Spectrum, $22, a light-as-air SPF that works brilliantly under makeup (and without). For your body, try Sun Bum Mineral SPF 50 Sunscreen Lotion, $15. It smells like vacation and soaks up in an instant.
Regarding lupus-related hyperpigmentation – which can be left behind after lesions begin to heal – Dr. Shamban says to reach for a brightening cream with hydroquinone (although always check with your doctor first as some people may be sensitive to this ingredient). Azelaic acid, kojic acid, niacinamide, and licorice extract are some great alternatives to hydroquinone, which should not be used if you are pregnant.
“Discolorations can [also] be treated with some laser or light therapies, but with careful consideration to inflammatory response. You should always check with your board-certified dermatologist [to see if you’re a candidate],” adds Dr. Shamban. “Lumpy, pitted scarring – or other residual scars – may be treated with some filler.”
If you’re seeking soothing skincare for lupus, look for products formulated with green tea, colloidal oatmeal, Centella Asiatica/tiger grass, or chamomile, which are skin-calming ingredients that can help reduce the look of redness.
 Source: Naturopathica, Dr. Jart
Source: Naturopathica, Dr. Jart
One of our faves is Naturopathica Gotu Kola Intense Repair Balm, $62, an unsuspecting pink-hued balm that soothes, locks in moisture, and strengthens the skin barrier. Dr. Jart+ Cicapair Tiger Grass Cream, $48, is another good one that’s a traditional cream formula versus balm.
 Source: Covergirl, L’Oreal
Source: Covergirl, L’Oreal
“[Finally], try adding in a mineral-based primer, ideally with some green tones to balance out redness. You can also try a serum-based foundation with anti-inflammatory ingredients built-in,” says Dr. Shamban. We like Covergirl truBLEND Base Business Face Primer, $8, and L’Oreal Paris Age Perfect Radiant Serum Foundation with SPF 50, $12.
We also love the natural and organic skincare brand, Beneath Your Mask, founded by Dana Jackson, who was diagnosed with Systemic Lupus Erythematosus (SLE) and Lupus Nephritis in 2011. In 2012, she created Beneath Your Mask’s first product, the Heal: Whipped Skin Soufflé, a nourishing soufflé-textured cream with anti-bacterial, anti-aging, and antioxidant properties that helps to hydrate and strengthen skin, maintain skin’s elasticity, reduce inflammation and protect skin cells from damaging free radicals. And, of course, it is most importantly safe and gentle for those with lupus or other skin sensitivities.
 Source: Beneath Your Mask
Source: Beneath Your Mask
Dana says on her brand’s page that she “Sought to create products that were safe, non-irritating, and non-toxic for the skin to absorb and that would not challenge the immune system.” The brand now has a whole collection of skin-soothing, effective products, from lip balm to face masks. Dana continued, “I strive to create the highest quality, most potent, non-toxic, all-natural, organic, vegan* products that actually work to hydrate the skin as well as feel and smell incredible for people all over the world.” Truly inspiring!
We know all the above is a lot to take in, but we hope that it helped you better understand lupus. If you suspect you might have lupus, reach out to your doctor and move through the steps that can either help eliminate it as a potential diagnosis, or set you on a path to proper management. No matter what, be good to your body and treat yourself with care from the inside out!
Disclaimer: Every product we review has been independently selected and tested without bias by our editorial team. We never take payment to review products, however, some brands allow affiliate links, so we may earn a commission if you purchase a product by clicking on one of our links.





















Leave a comment